Columbus Regional Hospital ExpansionVirtual construction & technology, Healthcare, Emerging technology, Lean Construction, Projects
You have a master plan, but do you have a maser model?
As healthcare providers experience the benefits of using building information modeling (BIM) at the project level, it’s becoming more common for them to make it a requirement that architects, engineers and contractors (AEC) use this technology on their projects. A recent survey of our subcontractors and our own results support this, as well as other industry case studies and research.
However, the largely untapped potential exists to extend those benefits past the project completion date and into the lifecycle of the facility. According to a 2015 Dodge Data & Analytics SmartMarket Report, “While over half of contractors (52%) frequently or always provide models to owners, only 17% of the owners surveyed are frequently or always using models for facility management.”
A recent white paper published by the Health Care Institute (HCI), shares the benefits of BIM for operations and facility management (FM), backed by examples from leading providers such as the Mayo Clinic and The Ohio State University Wexner Medical Center.
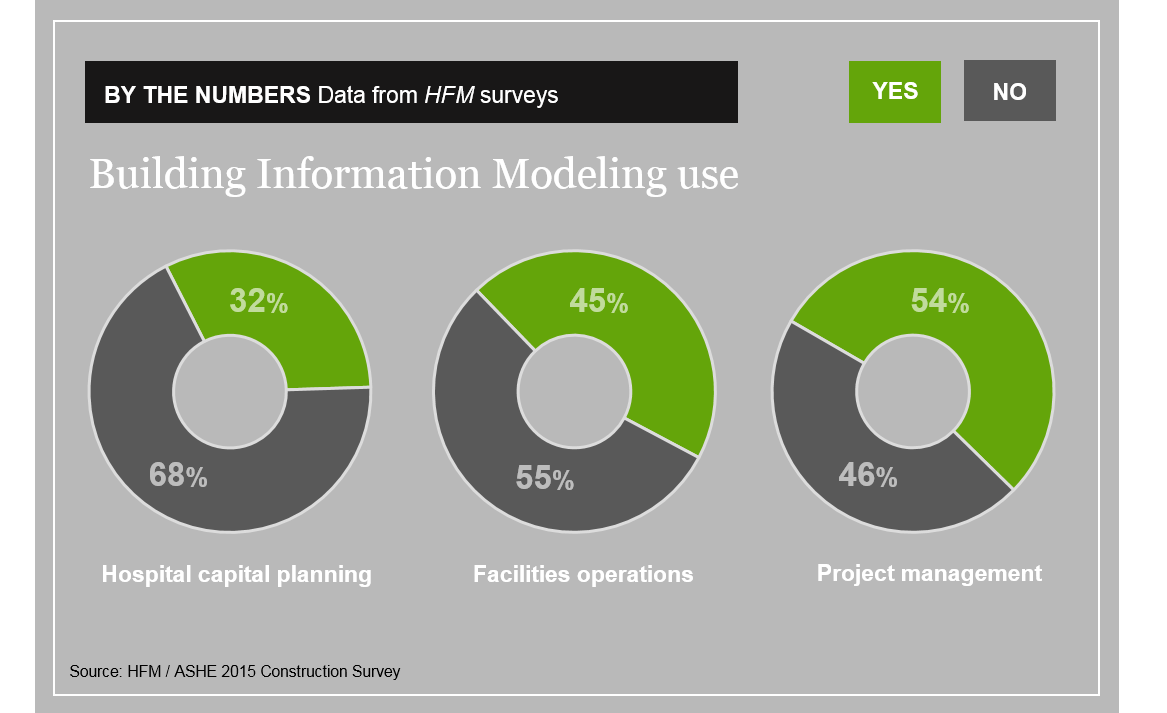
Clearly the healthcare industry is not capitalizing on all of the benefits that BIM offers. The graphic above references findings from the 2016 Hospital Construction Survey by Health Facilities Management. It shows the adoption rate for BIM declines as the data moves from a project, to facility management, to master planning.
In short, AEC teams are using BIM because it saves all project stakeholders time and money during design and construction. At the end of the project the models exist. But if the owner did not specify any requirements for how those models and the associated information is to be turned over to them at the end of the job, they are likely to receive models that met the needs for designing and constructing the now-completed project but are not optimized for use in facilities management.
What’s preventing the switch?
The steps of connecting BIM with facilities management can seem daunting to an owner. Processes are already in place. People are already trained to know how to access the information they need. It’s a change for the facilities operations staff. It’s a change for a design team. It’s a change for the construction team. They need a compelling reason to change.
The biggest observation I’ve made is that as a construction industry, we don’t have a true understanding of how the information we turn over is truly used once it leaves our hands. At the same time, many owners do not truly understand BIM workflows, how models are created and what information can be added into those models.
Once an owner, a designer and a contractor fully understand one another’s workflows, the possibilities become immediately apparent. The first step in making the switch…is starting the conversation.
Telling the story
The story of Columbus Regional Hospital is a story of an owner who started that conversation. It’s a story that tells how that conversation can turn into a rich understanding by all parties of how a model can be used through a facility’s lifecycle. It tells how a model can be used to drive predictable outcomes, and it proves that healthcare providers of all sizes can start planning now to implement a master model approach and leverage the information BIM can hold to more efficiently manage their facility.
Closing the gap
Those who are using BIM for facility management right now tend to be large institutions with the resources to support the work that is involved in making the switch. Columbus Regional Hospital does not fit that mold.
Even before making the switch to BIM, Columbus Regional Hospital was well organized with their data management, but they started to think about what happens when their keeper of the information leaves, the hospital's needs change or it's time to expand. With multiple file types, locations and sources of data, it was taking months for a dedicated person to cross-reference and update their system with new information once a project was completed.
Knowing that BIM was quickly becoming the new way of designing and building, they reached out to Hutton and Hutton Architects and Engineers to start asking questions about how they could capitalize on this technology to benefit operations of their facility.
Developing a solution
Once Hutton and Hutton had a good understanding of the hospital’s facilities operations, goals and desired outcomes, they started identifying standards for the development of a master model, how that master model would be updated during projects and what information would be populated into the model.
They wanted a master model that they could use as the source and standards for their operations. Steps would be eliminated, which would also reduce the potential for errors and omissions. Their vision was to have one prime model, where they could check relevant parts of the model out, update them with new information and check them back in as the new prime model.
The solution focused on the process first and technology second. It started with the development of architectural and structural models for their existing campus because of the anticipated challenges associated with their upcoming projects. It was designed for ease of use. BIM creates large file sizes that can be time-consuming to manage, both in terms of finding the data and working with it, so the prime model was constructed of smaller sub-models. It uses industry-standard COBie data for BIM and cross-references that to the Computerized Maintenance Management System (CMMS), with a total of 74 fields of information.
Validating the solution
We tend to think in silos within our own areas of expertise so I found the process that the hospital implemented to validate their solution particularly enlightening for me. And it was pivotal to a solution that worked….for everyone!
As the model was starting to be developed and the FM process was starting to come into focus, Columbus Regional Hospital invited Hutton & Hutton, MEP Engineer KJWW and Pepper to a two-day lean "value stream mapping" process to learn from each other.
Columbus Regional Hospital's director of facilities and materials management led the process. He wanted to know how the design and construction team develops the model and wanted the project team to understand how the hospital uses the data from the model for their campus operations – so that together we could develop a process to deliver the model and data in a way the hospital can use moving forward.
Throughout the day, he would ask: “Are we making this too complicated or isolating someone?” He wanted the model to work for everyone who will be using it.
As a result, several duplicate steps were eliminated and quality control stop-gates were added. For example, originally the plan was to have the engineers model the mechanical, electrical and plumbing systems, but after talking through how we use the model during construction, it was decided that we would use the shop drawings that were provided by the subcontractors instead.
Pepper has delivered specific facilities management solutions before, but this was different. The hospital didn't have a specific facilities management software in place. The solution was flexible to allow the hospital to choose its own software platform at a later date and specific enough to establish standards and processes that would work for all future projects.
Having the meeting upfront allowed Pepper to contribute solutions that worked for both current project challenges and the hospital’s operations because we had a new understanding of how they would be using the data.
The guidelines the hospital provided included descriptions and examples so we could request the specific information from contractors, delivered in a way that the hospital could use without editing or manual conversion.
Time to test the process
The process of developing a master model was aligned with hospital expansions and renovations that included a loading dock and utility tunnel, cancer center and emergency department, which became the test.
The project itself was far from simple. With existing utilities running under the site and construction occurring on all sides of the hospital, how the team planned and managed the details mattered to the hospital's current patients and their families. They needed every activity to result in predictable outcomes.
The project was delivered through a design-build contract, with design-assist MEP contractors. From our perspective, this helped us control how we used the model and allowed us to get the most benefit from implementing technology. The architect was able to take advantage of the campus master model to start their construction documents. The FM and modeling guidelines were communicated to subcontractors, and they were on board with the process.
We also gathered existing conditions as part of the project and added that information to the master model, further streamlining the model development process.
As I mentioned previously, the AEC industry’s shift to BIM is a big part of what led to Columbus Regional Hospital making the shift. Some of the ways we used BIM during design and construction included:
- Using design team and subcontractor models to ensure system coordination and constructability
- Using laser scanning to help with coordination of a new utility tunnel that ties into an existing tunnel – prefabricating the new systems, delivering and placing them from truck to tunnel. This saved two weeks off of the schedule and created a safer construction environment and higher quality end product.
- Scanning custom-fabricated existing light fixtures to create drawings for new fixtures that needed to match existing conditions exactly. Rather than going back to the original fixture fabricator, the team was able to bid this work out to multiple firms resulting in competitive pricing.
- Creating virtual and full-size mockups for users to test the space.
- Using the model to determine details and issues of new connections to the existing building.
At the end of the project, the models that were delivered to the client were not just what we thought would be the best for them to have. The models that were delivered met the client's expectations for a useful deliverable.
Tips for success
If I were to give advice to another client considering a FM solution, here’s what I would tell you from a contractor’s perspective:
- Start the conversation internally and leverage AEC resources for more information
- Start with the end in mind – how you will use the data?
- Think through the workflow process first before considering the technology
- Engage everyone who will use the model in the solution development process
- Identify where you can eliminate duplicate steps
- Think about a solution for who will manage the data ongoing
- Be flexible, ask questions, explore options
- Your roadmap to a comprehensive solution will be unique
Now it’s your turn
The HCI report that I referenced in the introduction concludes with the following challenge: “While use of BIM in facilities operations has risen in recent years, in most cases facilities departments are each creating their own processes for using BIM data. Each organization is starting from the beginning, rather than benefiting from knowledge sharing among organizations that have already put best practices in place.”
The possible solutions are endless and processes will be unique for each given facility. However, starting the conversation with partners in the AEC industry can help bring a solution into focus much quicker than you might think.
We accepted the challenge of knowledge-sharing last week when we joined Columbus Regional Hospital and Hutton & Hutton at the Midwest Healthcare Engineering Conference. Together, we presented this process and our keys to success. We hope to continue the conversation in the months ahead so others can learn from our experience.
If you have a question about how to get started or want to learn more, contact us. We would like to hear from you.
About the Author